AntiVEGF
- for wet ( exudative) form of AMD (age-related macular degeneration)
- for myopic macular degeneration
- for diabetic retinopathy
- for central retinal vein occlusion
What is wet (exudative) form of age-related macular degeneration (AMD)?
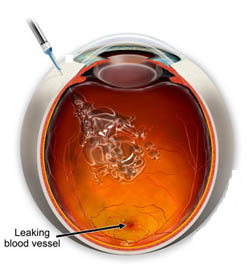
Wet or exudative form of age- related macular degeneration is less common type of AMD. Almost 90 % of patients diagnosed with AMD have the dry form, and only 10 % have a wet form of AMD.
Wet AMD occurs during the aging process, when the poor circulation in the body leads to ichaemia and consequently causes the lack of oxygen and nutrients to tissues. The body responds by creating new blood vessels, which should additionally supply the ischemic tissue. In the eye, they grow beneath the retina in the macular region and choroid develops CNV. These newly vessels are unstable, weak and thin-walled and prone to bleeding or "leak", and unfortunately , there is entirely the opposite effect. Liquid comes out through the thin walls of blood vessels and accumulates in the tissues, swelling (oedema) develops. Bleeding and exudation only further increase the ischemia which leads to further damage and scarring of the macula. This can cause a very rapid damage and even loss of the central vision.
The latest and most effective therapy of choroidal neovascularization ( CNV ) in AMD syndrome is antiVEGF therapy. Numerous studies have shown that anti VEGF medicines are effective in stopping the damage and improving vision in patients with the wet form of AMD.
What is myopic macular degeneration?
Pathological myopia is a special kind of myopia associated with the degenerative changes in the retina that can cause vision impairment.
Since the myopic eyeball is bigger, the retina is thinner and may develop microcracks at its basis (Bruch membrane). These cracks represent a stimulus for the formation of new blood vessels in the choroid of the eye and the development of CNV. This condition usually occurs beneath the macula , where the retina is the thinnest and the most fragile. These blood vessels are unstable, weak, thin-walled and prone to hemorrhage. Initially, lesions are short termed and usually pass spontaneously without a treatment, but if repeated, can lead to the formation of the pigmented scars. ( Fuchs' spots). Central vision is damaged, and there is an image distorsion called metamorphopsia, reduced sensitivity to colour and light. There is a poor prognosis regarding the visual acuity.
The latest and most effective therapy for CNV in myopia is an antiVEGF therapy. Referent studies have shown that antiVEGF medicines are effective in stopping the damage and improving the vision in patients with this pathological condition.
What is diabetic retinopathy?
Diabetic retinopathy is an eye disease that occurs in diabetic patients with poor glycemic control. Evolving over the years, exaggerating changes may cause severe visual impairment. Diabetic retinopathy is the result of damage to the walls of small blood vessels and microcirculation of the retina due to high blood sugar level. Result is damage caused by the hemorrhage and " leakage" of fluid from blood vessels and disposal of hazardous materials into the tissue of the retina. This is what causes poor nutritional status and lack of oxygen in the tissue, particularly a sensitive macula.
There are two forms of diabetic retinopathy (DR) :
Nonproliferative diabetic retinopathy is the beginning of the disease, when the injured artery of the retina and leak blood plasma elements occur as spotty bleeding, enlargement of capillaries ( microaneurysms ) , swelling and deposits of solid material caused by the poor diet and lack of oxygen in retinal tissu ( ischemia and hypoxia ) . The macular disease, especially sensitive to these changes, represented as a distortion of the image, difficulties while reading and loss of contrast ( diabetic maculopathy ) .
Proliferative diabetic retinopathy is a heavy degree of progression of diabetic eye disease when the massive ischemia generate new blood vessels ( neovascularization - NV ). Blood vessels are very weak and have thin walls which tend to leak fluid and blood. This results in swelling, exudates, increased bleeding in the retina and vitreous with a sudden and dramatic loss of vision.
Risk factors for severe visual impairment from DR :
- Unregulated blood sugar (HbA1c over 6.5 to 7 %)
- High blood pressure over 140 mmHg
- High levels of blood lipides
- Anemia The most severe forms of diabetic retinopathy is treated in the following way:
1. Timely laser treatment of the retina called photocoagulation ( LPC )
2. AntiVEGF therapy and vitreoretinal surgery
What is the occlusion of blood vessels in the eye?
Occlusion of blood vessels ( arteries and veins ) , as in other parts of the body that lead to for example heart attack develops stroke of the eye. It occurs to people who have problems with cardiovascular system, circulatory or blood clotting disorders. Often the result of thrombus formation, when a thrombus obstructing the lumen of the blood vessel and stops blood circulation. It can occur in the hypertension and atherosclerosis, where the arteries pressure the veins and disrupt the flow of blood through them. As a consequence, it leads to malnutrition and lack of oxygen in the tissue of the retina, resulting in ischemia and developing of the new blood vessels. These circumstances can develop very rapidly and emergence of neovascular glaucoma can become reality, and as a serious visual impairment can follow within 100 days.
Therapy is as follows:
1. Timely laser treatment of the retina called laser photocoagulation ( LPC), especially after central retinal vein occlusion ( CRVO).
2. AntiVEGF therapy
What is an antiVEGF therapy?
AntiVEGF medicines (anti- vascular endothelial growth factor ) are used to prevent creating more blood vessels - neovascularization in ischemic tissue. AntiVEGF medicines can stop the growth of new blood vessels, which significantly reduces the risk of bleeding, leakage, scarring and further vision loss.
Method of antiVEGF therapy application:
AntiVEGF medicines are given as an injection into the vitreous (corpus vitreum) . The injection is given through the sclera in the operating room under the sterile conditions. Local anesthetics are applied as drops and the procedure is painless. The needle used is very sharp, small and short. Just injecting drugs into the eye takes a few seconds and feels like a mosquito bite. After that, patients are advised to put eye drops for a few days as a prevention of the infection.
The treatment is to be repeated by the internationally recommended protocol. Checkups are obligatory until the condition is stable. Usually the first three doses are given monthly, then in six months and a year. The number of injections given will be determined by the ophthalmologist based on the findings and additional diagnostics. Medical examination to test vision and control OCT will compare the situation before and after treatment with antiVEGF therapy.
In Polyclinic MILMEDIC this therapy is applied with a great success, and Prof. Dr. M.Vukosavljevic MD PhD with his team and extensive experience is a guarantee of a superior treatment.
